CALL: 1-800-797-0361 (M-F 8AM-6PM EST)
The only true “fix” for a deviated septum is surgery, if it is successful. But, if you aren’t sure about undergoing surgery, or you are not ready to have surgery, there are alternatives to deviated septum surgery. Read on to learn more about your options.
“…of all of the nasal cones sold all over the internet and in stores, your Max-Air Nose Cones are the best nasal cones. My ENT doctor at Kaiser here in California told me about them. Thank you! ”
Alice S.
An Ear, Nose and Throat surgeon has diagnosed you with a deviated septum. Now you want to know if surgery is the only option to fix it, or if there are alternatives to relieve the airway obstruction without surgery.
It is normal to find out as much as you can about your diagnosis of septal deviation before deciding to undergo nasal surgery.
Whether you are considering septoplasty surgery or not, it makes sense to research the risks and costs, to decide if alternatives to deviated septum surgery are worth trying first.
Depending on the severity of the deviation, nasal surgery may be helpful or necessary to correct the deviation to the nasal septum. But how do you know if surgery is the best option for you? To make that decision, it makes sense to do a little research into the procedure and learn what is involved.
Since, you may decide instead to try an alternative to deviated septum surgery, we did a little research and compiled a list to help you.
Here is a list of the top 8 things to know before deviated septum surgery:
1) Surgery to correct a deviated septum is a septoplasty.
The medical dictionary cites the origin of the word septoplasty as septo, from Latin “sepes” meaning hedge or wall to divide, and plasty meaning to mold, graft or form a specified part of the body. It is the surgery that corrects or straightens abnormalities or damage to the nasal septum.
2) An Otolaryngologist (Ear, Nose & Throat, or ENT Surgeon) performs the septoplasty.
The surgeon repairs the nasal septum (the cartilage) in the center of your nose that “divides” the nasal airways. Each surgeon decides how best to repair or straighten the deviation. There are two types of surgery that they perform, open and closed septoplasty. The decision to perform an open or closed septoplasty depends on the location of the deviation and the degree of deviation to the septum.
The goal of the surgery is to improve breathing by removing the nasal obstruction from the deviation to the septum.
3) Septoplasty is performed under general anesthesia at an outpatient facility.
There is some controversy about classifying septoplasty as outpatient surgery, because like any surgery complications can occur.
The primary complication for septoplasty is excessive bleeding, which requires hospitalization. According to this research study, hospitalization is required more than 8% of the time for complications due to septoplasty surgery. This is higher than typical outpatient surgery. Typical outpatient surgery is classified as having a 2% to 3% incidence of hospitalization for any complication.
4) Undergoing septoplasty to improve the appearance of your nose, rather to improve your breathing, is elective surgery, and is not covered by insurance.
Usually a deviated septum isn’t very noticeable and doesn’t effect your appearance. In other cases, a deviated septum is quite evident and causes the face to look asymmetrical, or misshapen.
If the deviation affects your appearance, you may choose to undergo the surgery to straighten your nose so that you look better. Undergoing surgery to look better is cosmetic surgery. Cosmetic surgery is elective surgery, (versus functional), and, as a consequence, is not covered by insurance.
5) For insurance to cover septoplasty, your doctor has to determine that it is medically necessary.
In order to determine the medical necessity of surgery, your doctor will document your airway obstruction and breathing discomfort. The ENT will test your airway function and notate the degree of nasal impairment. Then you will have to try prescribed alternative treatments to relieve the obstruction.
If breathing discomfort and nasal obstruction are not improved by these treatments, then surgery may be deemed medically necessary and covered by insurance. Check with your insurance carrier for the specific requirements of your policy.
6) Costs for septoplasty can range from $4K to $14k depending on who performs your surgery and your geographic location.
If your insurance will cover your surgery, you will need to speak with your insurance company to determine what your deductible will be and if there are any out-of-pocket expenses that will be necessary for your recovery.
7) The deviated septum repair surgery normally takes 30 to 90 minutes and recovery, without complications, usually requires 1 to 2 months.
8) Potential complications and the most common risks of septoplasty surgery are:
- unresolved symptoms of nasal obstruction,
- the nasal septum may “revert” or return to its original deviated position or become worse
- difficult healing resulting in soft tissue collapse or scarring inside the nose
- excessive bleeding
It appears that there are many disadvantages to undergoing this surgery. And there are. But, surgery also offers a big advantage. It is the only way to truly fix a deviated septum because it surgically repairs the septal deviation. And, when successful, it is a long-lasting fix.
What is the success rate of deviated septum surgery?
According to published research in medical journals, the success rate of primary nasal deviated septum surgery is 43% to 85%. These percentages indicate that 15% or more patients have unsuccessful outcomes after one surgery.
In one large research study, it was reported that 48% of patients needed a second surgery, called revision septoplasty to successfully relieve the symptoms of nasal obstruction. As a consequence, the estimate is that potentially 50% of patients can have unresolved obstruction after surgery.
Does a Deviated Septum Need to be Fixed?
After reviewing the risks and considering the options, does a deviated septum always need to be fixed?
If your deviated septum symptoms are severe and significantly compromise your health, surgery is generally your only option. But, if symptoms or discomfort are minor you may not require surgical treatment, and there are definitely less risky and less expensive options to try first.
Deciding to have surgery is a very personal health decision and should be thoroughly discussed with your doctor. The risks of surgical treatment can often outweigh the benefit. If you are risk averse, consider our alternatives.
What are the alternatives to surgery for a deviated septum ?
Because age, other health issues, cost, risks or inconvenience can eliminate surgery as a solution, you may have to consider alternative solutions.
If you are not a candidate for nasal septum surgery, Max Air Nose Cones are a great alternative. They are soft and flexible. They comfortably conform to the deviation of the septum, and hold the airway open around the curved portion of the nasal septum. Their unique design and ergonomic shape deliver comfortable, convenient breathing relief without the need for nasal surgery.
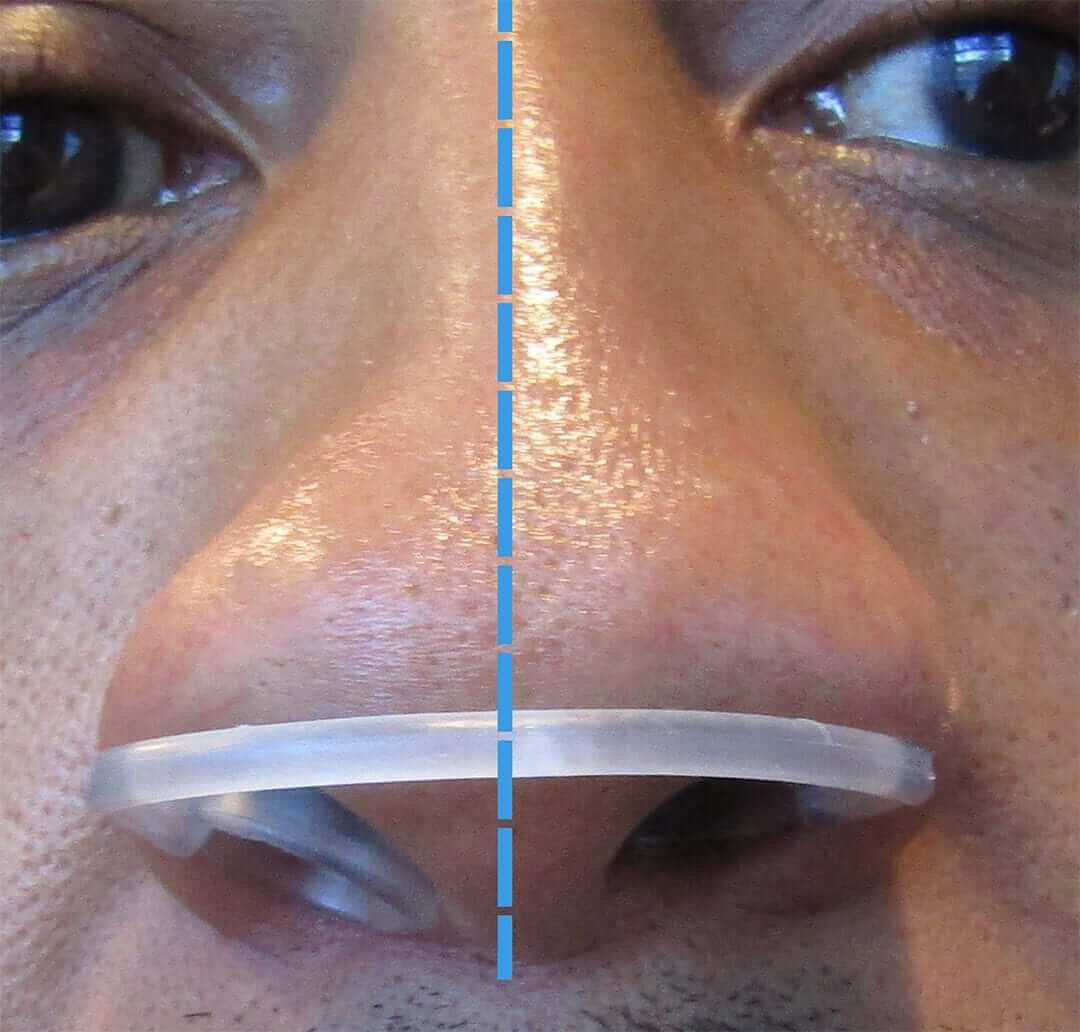
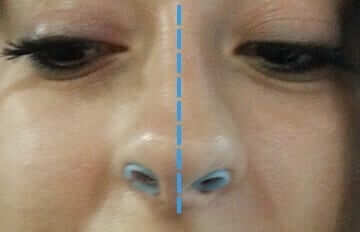
As illustrated in these photos, the Max-Air Nose Cones adapt to the asymmetry of the nose caused by the deviation to the septum.
How can I immediately improve my breathing comfort with a deviated septum?
The reason that it is difficult to relieve a deviated septum through medical management (by using nasal sprays or oral decongestants) is that the nasal obstruction is an anatomical abnormality. This means that it is part of the physical structure of your nose, sort of like crooked teeth.
A fall or damage to your nose from playing sports is the most common cause of a deviated septum. Another common cause of a deviated septum is due to incorrect developmental growth of the airway from childhood.
Poor airway development as a child is referred to as pathological septal deviation. Pathological deviated septum is usually the result of mouth breathing.
Medical research estimates that 80% of the population has some level of deviation to their septum. Septal deviation is very common.
Because septal deviation is so common, there are a variety of nasal devices made to relieve the airway restrictions. Many of these devices are uncomfortable, because they are poorly engineered and made with the wrong materials. It is important that the device is soft and ergonomically engineered for comfortable airway relief.
Max-Air Nose Cones are soft and great time was spent engineering them so so that they do not irritate the airway. The soft flexible material gently holds the airway open and clears a breathing pathway around the area where the septum is deviated.
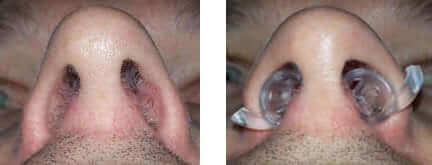
Max-Air Nose Cones are an easy-to-use alternative to surgery.
The above commentary represents the opinions of our experts. This website content is only informational and is not medical advice. An Ear, Nose and Throat surgeon provides medical advice for nasal obstruction. Seek their counsel for decisions about nasal surgery, breathing and nasal health.







